Virtual Intervention
Treatment of IAs have generally taken one of two paths: Either clamping off the blood flow, or stenting with a meshed-tube-like device. The stent can either provide a scaffolding for coils to fill the IA sac, or, more recently, it can functionally modify blood flow near the IA orifice, with the goal being the elimination of the IA. This works by reducing blood inflow to the IA dome, and thus without coils can attenuate the flow activity inside the IA, inducing a thrombotic process of occluding the IA. Since the functionality of this so-called “flow diverting” strategy largely relies on hemodynamic modification of specific stents, computational fluid dynamics (CFD) should prove to be very helpful in unveiling the nature of aneurysmal flow change which is closely related with the thrombogenesic process.
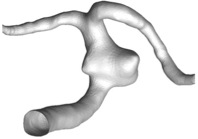 A series of studies have been conducted in our group using patient-specific aneurysm models (see left figure) to evaluate the flow-diverting efficacy of different stent designs and applications. First, for each CFD case, laser-cut, designed-for-scaffolding stents were geometrically implanted across the IA region either alone or in a combined manner. CFD analyses then provided hemodynamic information about flow pattern, vorticity, low wall shear stress (WSS) area, wall pressure and flow turnover time inside the IA. This allows us to identify the preferred stent combinations as well as positioning strategies that are more likely to produce optimal IA flow alterations.
A series of studies have been conducted in our group using patient-specific aneurysm models (see left figure) to evaluate the flow-diverting efficacy of different stent designs and applications. First, for each CFD case, laser-cut, designed-for-scaffolding stents were geometrically implanted across the IA region either alone or in a combined manner. CFD analyses then provided hemodynamic information about flow pattern, vorticity, low wall shear stress (WSS) area, wall pressure and flow turnover time inside the IA. This allows us to identify the preferred stent combinations as well as positioning strategies that are more likely to produce optimal IA flow alterations.
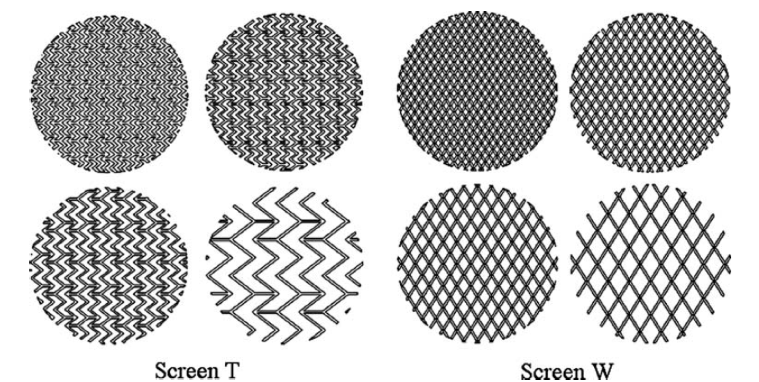
Next, we explored several design parameters of flow diverting stents via CFD examination. Stents with different porosities, geometrical patterns and strut cross section shapes, were evaluated based on the WSS manipulation and resultant hydraulic resistance of each stent model. The figure below shows the mesh pattern for two different brands with their various porosities.
Finally, we have adopted a new method of simulating the clinical deployment process of flow diverting stents to obtain more realistic configurations and positioning versus geometrical implantation called HiFiVS (high-fidelity virtual intervention). This deployment modeling technique has been applied to one recently developed flow diverter designed to divert IA blood inflow and induce curative artery reconstruction. The unique woven structure design of the flow diverter (FD) makes its deployed configuration based more on the clinician’s operation, and is difficult to predict without mechanical simulation of the process.
Further Reading:
Tremmel M, Xiang JP, Natarajan SK, Hopkins LN, Siddiqui AH, Levy EI, Meng H, "Alteration of intraaneurysmal hemodynamics for flow diversion using enterprise and vision stents". World Neurosurgery. 2010;74:306-315. PMID: 21197155
Kim M, Levy EI, Meng H, Hopkins LN, "Quantification of hemodynamic changes induced by virtual placement of multiple stents across a wide-necked basilar trunk aneurysm". Neurosurgery. 2007;61:1305-131. PMID: 18162911
Kim M, Taulbee DB, Tremmel M, Meng H, "Comparison of two stents in modifying cerebral aneurysm hemodynamics". Annals of Biomedical Engineering. 2008;36:726-741. PMID: 18264766
Ma D, Dargush G, Natarajan SK, Siddiqui AH, Meng H, "Computer modeling of deployment and mechanical expansion of neurovascular flow diverters in patient-specific intracranial aneurysms". Journal of Biomechanics. 2012;45:2256-63. PMID: 22818662